ATLAS research gives new insight into liver fibrosis
Inflammation and scar tissue in the liver can lead to cirrhosis and liver cancer, yet no efficient treatment is available today. A research team from the Center of Excellence ATLAS at the University of Southern Denmark has gained new insight into the process behind the transition from a healthy liver to an inflamed one with scar tissue. The new information was recently published in the scientific journal Hepatology and can lead to better diagnosis and treatment of liver diseases in the future.
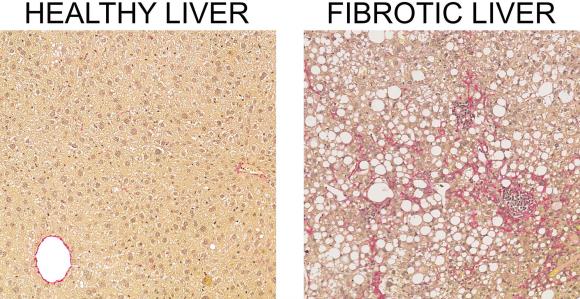
The liver is one of the overlooked organs of the human body, but it is also one of the most hardworking ones. It ensures several vital functions, such as controlling our digestion; regulating our sugar metabolism; controlling our immune system; and detoxing alcohol. The liver is thus a steadfast organ that we can’t live without, and if damaged, it can become inflamed and develop scar tissue, also known as liver fibrosis.
The global prevalence of both liver inflammation and liver fibrosis has taken on pandemic proportions, but still no effective treatment is available. Liver fibrosis may develop into cirrhosis and liver cancer. A research team from the DNRF’s Center for Functional Genomics and Tissue Plasticity (ATLAS) at the University of Southern Denmark has gained new insight into the cellular processes that occur when a healthy liver develops into a liver with inflammation or scar tissue. The study was done with laboratory mice, but according to the researchers from ATLAS, the results may also be transferred to humans.
“In the mice we found some key genes that precisely follow the development of fibrosis, and these genes now also turned out to be useful diagnostic markers for fibrosis in humans,” said Kim Ravnskjær, associate professor at ATLAS and senior author behind the study.
The results are based on microscopy examinations with a very high resolution of liver biopsies that the researchers took both prior to and 18 months after the operation on the mice. This was done in order to observe what type of liver cells and genes changed and how the cellular process unfolded in detail.
“In the future, naturally it would be more interesting if we could use the markers in a blood sample and discover fibrosis earlier on and more efficiently than today,” said Professor Ravnskjær.
Read more about the study from ATLAS in a press release from the University of Southern Denmark here
